Goa is abuzz with excitement as vintage bike and car owners, users, collectors and fans are decking […]
THE WAR AGAINST TB Yes, we can end TB… By Dr Amit Dias
Mar 21- Mar 27, 2026, MIND & BODY, HEART & SOUL March 19, 2026ON the occasion of World TB Day, observed on March 24, the global call—“Yes, We Can End TB”—serves as a powerful reminder that tuberculosis elimination is within reach through early diagnosis, effective treatment, and strong public health systems. In this interesting feature we address some of the most frequently asked questions to enhance understanding of this major public health challenge. “Many patients continue to seek care late due to lack of awareness. This article aims to bridge that gap by taking accurate, evidence-based information on TB to every household,” says Dr Dias.
What is Tuberculosis and what causes it?
Tuberculosis is an infectious disease caused by the organism Mycobacterium tuberculosis. It primarily affects the lungs (pulmonary TB) but can also involve other organs such as the brain, lymph nodes, spine, kidneys, and abdomen (extra-pulmonary TB). The disease is characterized by chronic inflammation and tissue destruction if left untreated.
How does TB spread? Is it highly contagious?
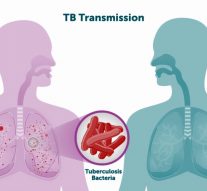
TB spreads through the air when a person with active pulmonary TB coughs, sneezes, or speaks, releasing infectious droplets. Individuals in close and prolonged contact are at higher risk. However, TB does not spread through sharing food, utensils, or casual contact. Infectivity reduces significantly after initiation of effective treatment, typically within a couple of weeks.
When and who discovered TB?
The causative organism of TB was discovered in 1882 by Robert Koch. This discovery established TB as an infectious disease and paved the way for diagnostic and therapeutic advancements. World TB Day is commemorated on March 24 each year to mark this milestone.
What are the common signs and symptoms of TB?
The clinical presentation varies depending on the site of disease. Pulmonary TB commonly presents with a persistent cough lasting more than two weeks, fever (often with evening rise), weight loss, fatigue, chest pain, and sometimes hemoptysis (blood in cough). Systemic symptoms such as night sweats and anorexia are also common.
Extra-pulmonary TB may present with lymph node swelling, bone pain, neurological symptoms, or abdominal complaints depending on the organ involved. For clinicians, a high index of suspicion is essential, especially in endemic settings. At our health settings we test for TB even if the cough is for less than 2 weeks in those who are at higher risk of developing TB.
What should a person do if they have symptoms suggestive of TB?
Anyone experiencing symptoms suggestive of TB should seek medical evaluation at the nearest health facility without delay. Early diagnosis is critical to prevent disease progression and transmission. Under NTEP the national program, diagnostic services and treatment are provided free of cost even at the primary health centers. All health care staff are trained in the early detection of TB and will be able to support you through the diagnosis and treatment phase of the disease. We will also take care of your supplementary nutrition. Individuals can also access guidance through the TB helpline (Nikshay Sampark: 1800-11-6666).

How is TB diagnosed in modern clinical practice?
The diagnosis of TB has advanced several fold in the recent years with the use of advance technology. TB is confirmed by demonstrating the presence of the bacterium in clinical specimens. Sputum examination remains a key diagnostic tool for pulmonary TB. In recent years, molecular tests such as nucleic acid amplification tests (NAAT), including CBNAAT, have become widely available. These tests offer rapid and accurate detection and can identify drug resistance, particularly to rifampicin. Extra-pulmonary TB often requires additional investigations such as imaging, histopathology, or cytology depending on the site.
Is TB curable? What is the duration of treatment?
Yes, TB is completely curable with appropriate treatment. Drug-sensitive TB is typically treated with a standardized regimen of first-line drugs over six months. Drug-resistant TB requires longer and more complex regimens. Adherence to the full course of treatment is critical; interruption can lead to relapse and development of drug resistance.
What are the complications of untreated TB?
Untreated TB can result in severe complications. In pulmonary TB, progressive lung damage can lead to chronic respiratory disability. Disseminated forms such as miliary TB can be life-threatening. TB of the spine can cause deformities and neurological deficits, while TB meningitis can result in long-term neurological impairment or death. Early diagnosis and uninterrupted treatment are the key to preventing these outcomes.
Can TB affect organs other than the lungs?
Yes, TB can involve almost any organ in the body. Extra-pulmonary TB commonly affects lymph nodes, pleura, bones and joints (especially the spine), abdomen, genitourinary system, and the central nervous system. While these forms are generally less infectious, they contribute significantly to morbidity and require specialized diagnostic approaches.
Who is at higher risk of developing TB?
While TB can affect anyone, certain groups are at higher risk. These include individuals in close contact with TB patients, people living in overcrowded conditions, those with compromised immunity such as HIV infection, individuals with diabetes, malnutrition, or those on immunosuppressive therapy. Smoking and certain occupational exposures also increase susceptibility.
How are TB and conditions like HIV and diabetes related?
Under the program we give special emphasis to diabetes and HIV. HIV is the strongest risk factor for progression from latent TB infection to active disease due to immune suppression. Similarly, diabetes increases the risk of developing TB and is associated with poorer treatment outcomes. Integrated screening and management of TB with these comorbidities are essential components of modern TB care.
Are health centres in Goa equipped to diagnose and treat TB?
Yes. Health facilities across Goa are well-integrated into the national TB programs and provide free diagnostic and treatment services. Molecular diagnostic facilities, trained healthcare personnel, and standardized treatment protocols ensure high-quality care. Both public and empanelled private providers contribute to TB care delivery.
What is the National Tuberculosis Elimination Programme (NTEP)?
India’s TB response is led by the National Tuberculosis Elimination Programme (NTEP), implemented under the Central Tuberculosis Division. The program focuses on early detection, universal drug susceptibility testing, patient-centric care, and robust monitoring systems. India has set an ambitious target to eliminate TB by 2025, ahead of the global goal of 2030. The initiative was earlier called NTCP and later RNTCP.
What new initiatives support TB elimination in India?
Several innovative strategies have been introduced under NTEP. The Nikshay digital platform enables real-time patient tracking and ensures continuity of care. The Nikshay Poshan Yojana provides financial support for nutrition during treatment. The Nikshay Mitra initiative encourages community participation to support TB patients. Active case finding and targeted screening in high-risk populations are also key components of the program.
What role do healthcare workers play in TB elimination?
Doctors, nurses and paramedics are central to TB control efforts. Their role extends beyond diagnosis and treatment to include counselling, ensuring treatment adherence, contact tracing, and infection control. Effective communication helps reduce stigma and improves patient outcomes. Healthcare facilities must also adopt infection prevention practices to minimize transmission.
How can TB be prevented at the community level?
Prevention of TB relies on early detection and complete treatment of cases. Improving nutrition, reducing overcrowding, and promoting respiratory hygiene are important measures. Public awareness and reduction of stigma encourage timely health-seeking behaviour. Screening of high-risk groups further helps in early identification and prevention of spread.
Conclusion
Tuberculosis remains a challenge, but it is one that can be overcome. With scientific advances, strong public health programmes, and active community participation, the goal of a TB-free India is within reach. On this World TB Day, let us reaffirm our commitment to early detection, complete treatment, and compassionate care for all those affected.
















