Goa is abuzz with excitement as vintage bike and car owners, users, collectors and fans are decking […]

HIDDEN NO MORE Finding the Undiagnosed, Supporting the Unseen! By Dr Amit Dias, MD
May 09- May 15, 2026, MIND & BODY, HEART & SOUL May 8, 2026A World Thalassemia Day Special
“NO child with thalassemia should struggle for blood in a world full of healthy people,” says Dr Amit Dias. World Thalassemia Day is observed on May 8. This article demystifies the complexities of the genetic blood disorder and explains how everyone can help….
EVERY few weeks, children with thalassemia quietly walk into hospitals for blood transfusions that keep them alive. Their lives revolve around blood counts, transfusions, medicines and hospital visits. Many grow up learning medical terms before they learn algebra. Yet despite affecting thousands of families across India, thalassemia often remains hidden in plain sight — undiagnosed, misunderstood, and under-discussed.
This year, World Thalassemia Day focuses on a powerful and much-needed theme: “Hidden No More: Finding the Undiagnosed. Supporting the Unseen.” The campaign draws attention not only to patients living with severe disease, but also to millions of individuals who unknowingly carry the thalassemia gene and may discover it only during marriage, pregnancy, or after the birth of an affected child.
Thalassemia is an inherited blood disorder in which the body cannot produce adequate normal hemoglobin — the protein in red blood cells responsible for carrying oxygen throughout the body. As a result, patients develop chronic anemia, fatigue, weakness, poor growth, and multiple long-term complications.
There are two major forms of the disease — “alpha thalassemia” and “beta thalassemia” — depending on which globin chain is affected. Beta thalassemia is more common in India. The condition can range from a mild carrier state, known as thalassemia trait or thalassemia minor, to thalassemia major, the most severe form requiring lifelong treatment.
India carries one of the world’s highest burdens of thalassemia. More than 100,000 people are estimated to be living with thalassemia major, and nearly 10,000 to 15,000 babies are born every year with the disorder. Around 3–4% of the Indian population are carriers of the thalassemia gene — amounting to nearly 40 million people.
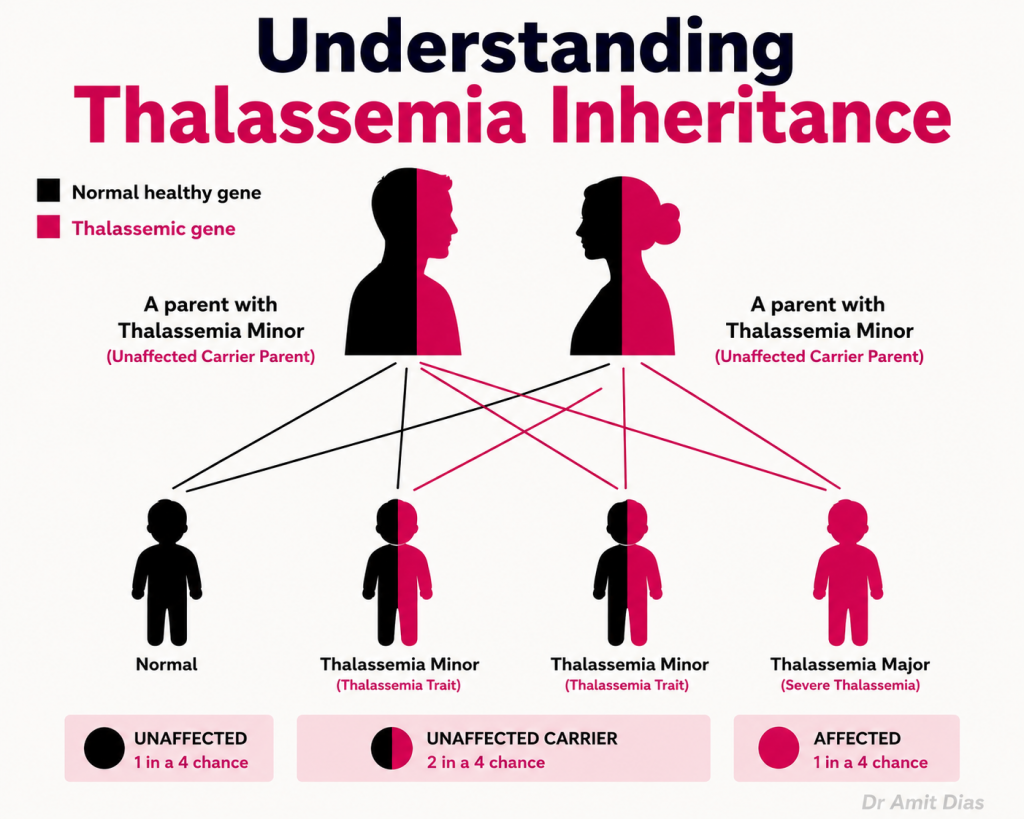
But what exactly does being a “carrier” mean?
A carrier usually has only one defective gene and is generally healthy. Many may have mild anemia or no symptoms at all and continue their entire lives without realizing they carry the gene. However, when two carriers marry, there is a significant chance that their child may inherit thalassemia major. This is why screening before marriage or pregnancy is so important. A simple blood test can identify carriers early and help families make informed decisions.
The 2026 theme strongly emphasizes “finding the undiagnosed” — because many people continue to live with silent or mild forms of thalassemia, without ever being tested. In many parts of India, routine screening is still not widely practiced, awareness remains limited, and diagnosis is often delayed. Unfortunately, by the time some patients are diagnosed, complications may already have begun.
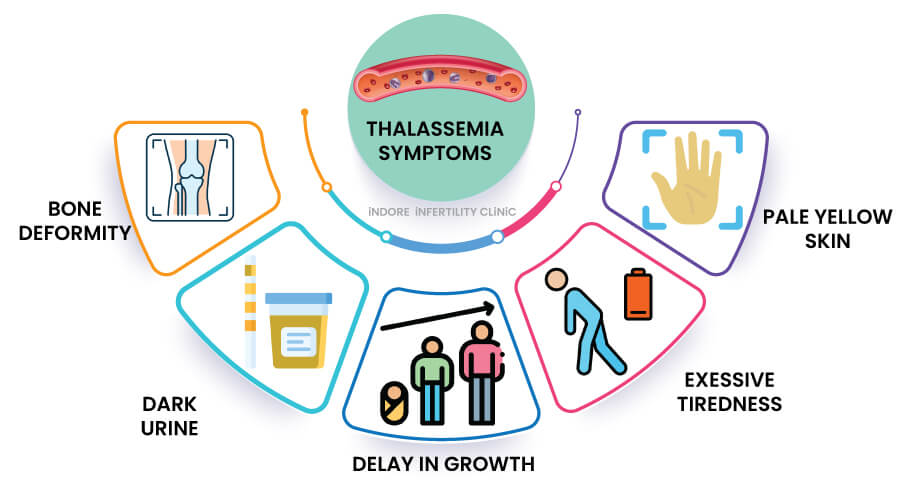
Children with thalassemia major usually begin showing symptoms within the first two years of life. They may become pale, weak, irritable, and fail to gain weight properly. Without treatment, severe anemia can affect nearly every organ system in the body.
The complications of thalassemia can be devastating. Chronic anemia places tremendous stress on the heart and other organs. Children may develop delayed growth, delayed puberty, weak bones, enlargement of the liver and spleen, and deformities of the facial bones due to excessive bone marrow activity. Repeated illness, poor school attendance, and emotional stress can affect academic performance and mental health.
One of the most serious complications is iron overload.
Patients with thalassemia major require regular blood transfusions — often every 2 to 4 weeks — to maintain adequate hemoglobin levels and survive. While these transfusions are lifesaving, each unit of blood contains iron. Unlike some other substances, the human body has no natural mechanism to remove excess iron efficiently. Over time, iron accumulates in vital organs such as the heart, liver, pancreas, and endocrine glands.
This iron overload can become dangerous and even fatal if not treated properly. Excess iron damages tissues and may lead to heart disease, liver failure, diabetes, thyroid disorders, infertility, osteoporosis, and growth disturbances. In fact, cardiac complications due to iron overload remain one of the leading causes of death in untreated or poorly managed thalassemia patients.
Fortunately, modern medicine offers a way to combat this problem through iron chelation therapy. Chelation medicines bind excess iron and help remove it from the body through urine or stool. Earlier, chelation therapy involved painful injections administered over several hours. Today, oral chelation medicines have improved convenience and quality of life for many patients. However, treatment must be regular and closely monitored.
Managing thalassemia therefore involves much more than blood transfusions. Patients require lifelong follow-up, careful monitoring of iron levels, cardiac evaluation, liver assessment, hormonal monitoring, vaccinations, nutritional support, and psychological care. It is a physically, emotionally, and financially demanding journey not just for the patient, but for the entire family.
The emotional burden is often overlooked. Children with thalassemia may feel isolated because of repeated hospital visits and limitations in daily activities. Parents frequently experience anxiety, exhaustion, and financial strain. This is precisely why the second part of this year’s theme — “Supporting the Unseen” — is so important. Beyond medicines and transfusions, patients need understanding, inclusion, emotional support, and dignity.
In Goa, the burden of thalassemia is very real. The GOTQoL (Goa Thalassemia Quality of Life) Study conducted by Dr Ankusk, Dr Mimi Silveira, Dr Amit Dias along with students Joachim and Yash, and published in the International Journal of Contemporary Pediatrics, highlighted the significant physical, emotional, social, and academic challenges faced by children living with thalassemia major in Goa. The study demonstrated that children receiving proper chelation therapy and strong family support had better physical functioning and improved quality of life outcomes.
The encouraging news is that thalassemia care has improved dramatically over the years. With modern transfusion protocols, safer blood banking practices, and better iron chelation therapy, many patients today survive well into adulthood and pursue education, careers, and family life.
Even more exciting are the possibilities emerging for the future.
Bone marrow transplantation, also known as stem cell transplantation, already offers a potential cure for selected patients when a suitable donor is available. However, the procedure is expensive and not accessible to everyone.
Newer therapies are now transforming the future of thalassemia care. Gene therapy aims to correct or replace the faulty gene responsible for the disease. Scientists are also exploring gene-editing technologies such as CRISPR, which may allow doctors to directly repair defective genes. Some patients treated in international trials have already achieved transfusion-free lives, offering hope that thalassemia may one day become curable on a larger scale.
Despite these advances, prevention remains the most powerful strategy.
Countries such as Cyprus and Iran have dramatically reduced thalassemia births through nationwide carrier screening and genetic counseling programs. India too has the potential to achieve similar success through awareness, premarital screening, prenatal diagnosis, and accessible testing services.
Importantly, thalassemia is recognized as a benchmark disability under the Rights of Persons with Disabilities Act, 2016 ensuring support for education, employment, and healthcare access for affected individuals.
This World Thalassemia Day, the message is clear: no patient should remain hidden, undiagnosed, or unsupported. In a world full of healthy people, no child with thalassemia should struggle to get blood. We must create communities that encourage screening without stigma, support patients with compassion, and ensure that every affected child receives timely care.
Because, sometimes, a simple blood test today can prevent a lifetime of suffering tomorrow.















